Until the end of March had the 32nd largest number of COVID-19 cases among OIC member countries, with as low as 51 confirmed cases. While a low number of infections may imply a good situation, healthcare experts warned that there could be many undetected cases in the country with nearly 165 million inhabitants. As testing for new cases increased in April after the South Asian country received testing kits and other medical supplies from Alibaba Group the number of coronavirus patients increased exponentially. With 4,998 confirmed cases, Bangladesh had the 9th largest number of COVID-19 patients among OIC countries as of 25 April 2020.
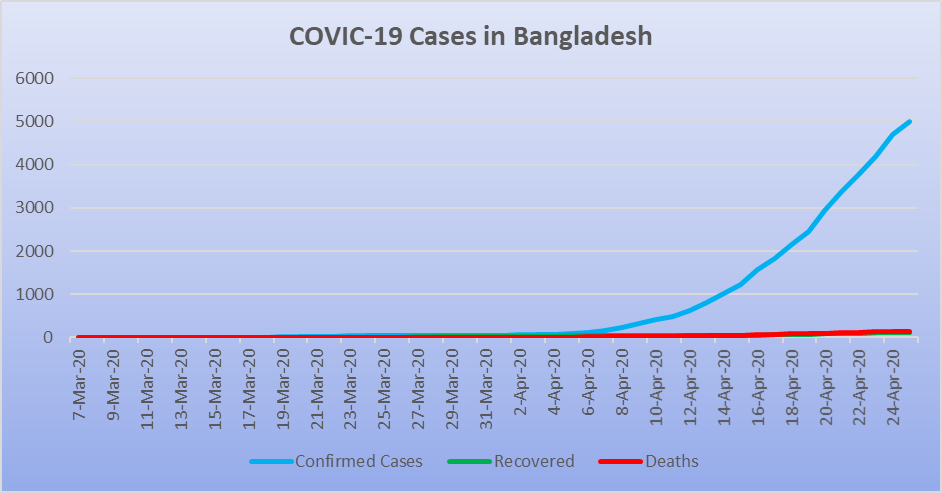
The drastic increase in coronavirus infections poses a critical threat to the country’s healthcare system; not to speak about the devastating impacts on its economy. Unlike most countries around the world, Bangladesh recorded more deaths than recoveries of COVID-19. Within the OIC countries, besides Bangladesh, only Somalia had more deaths than recoveries as of 25 April. This, coupled with the fact that hundreds of doctors and nurses have been infected by the highly contagious virus, reflects the seriousness of the conditions in Bangladesh.
On 23 April, the Bangladesh Doctors Foundation said that at least 251 doctors had tested positive for coronavirus, attributing the high figure to the lack of personal protective equipment (PPE) which makes medical staff more vulnerable to catch the virus from the patients who are being treated at hospitals. A study by BRAC University in Bangladesh found that about 25 per cent of doctors and nurses, and 60 per cent of medical support staff, engaged in treating coronavirus patients have yet to receive PPE.
Although most countries around the world suffer severe shortages of PPE and other medical equipment, a country like Bangladesh, with an already fragile healthcare system and low public awareness of the COVID-19 risks, could experience far more catastrophic consequences than other countries. To visualise this imagine the following scenario. Once a doctor is infected with coronavirus, he or she is quarantined and the hospital ward where they worked is shut for safety measures.
The damage, in this case, is threefold! First, it is related to the doctor’s health and safety which could have been protected had PPE been available. Second, the closure of some parts of a hospital wastes scarce resources. Third, it reduces the number of experienced doctors who could be treating other patients, especially knowing that the number of infections increases rapidly each day. According to the World Bank's development indicators in 2017, there was only one doctor for every 2,000 people in Bangladesh, one of the lowest ratios in the world.
Speaking of public awareness of COVID-19 risks, and how people could play a significant role in curbing the spread of the virus, Bangladesh has unique circumstances where many people tend to hide medical symptoms or any information related to the coronavirus to avoid stigma, social isolation or quarantine. Furthermore, enforcing social distancing in a crowded city like Dhaka, where people live in slums, is definitely a tough task. Quite the contrary, some people hide their COVID-19 symptoms to get treatment at hospitals that do not treat coronavirus patients.
The ignorance of those people could be much more harmful than they could imagine. One of the worst scenarios is that those untested people would infect doctors and other people at the hospitals that are not designated to deal with COVID-19 cases. This lead back to the main problem in Bangladesh at the moment represented in the increasing number of coronavirus infections among doctors, nurses and medical workers.
- Business News 100
- Country News 16
- Feature News 30
- International News 154
- Interview News 36
- National News 21